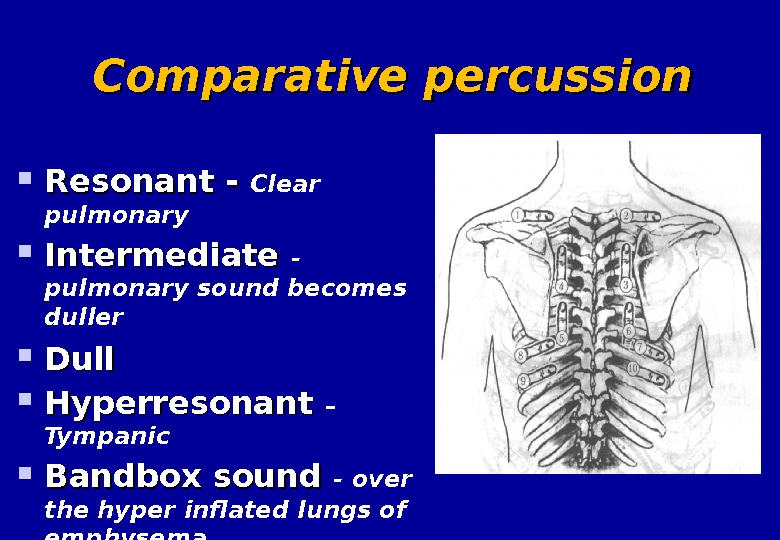
Palpate any abnormal masses or structures on the front and back of the chest.Bruises may indicate a fractured rib, and tenderness between the ribs may indicate inflamed pleura. To assess areas of tenderness, palpate areas of pain, bruises, or lesions on the front and back of the chest.During palpation, the physician checks for areas of tenderness, abnormalities of the skin, respiratory expansion and fremitus. Palpation is the use of physical touch during examination. The physician then typically inspects the fingers for cyanosis and clubbing. During intercostal retractions, the skin between the ribs appears to sink in as the intercostal muscles (the muscles between the ribs) aid in respiration. During supra-sternal retractions, the skin of the neck appears to sink in as the accessory breathing muscles of the neck contract to aid with inspiration. During a chest retraction, the patient's skin appears to sink into the chest. Chest retractions may be observed in patients with asthma.Cheyne-Stokes respiration may be observed in newborn babies, but this is occasionally physiological (normal). Cheyne–Stokes respiration is a breathing pattern consisting of alternating periods of rapid and slow breathing, which may result from a brain stem injury.Rapid breathing helps the patient compensate for the decrease in blood pH by increasing the amount of exhaled carbon dioxide, which helps prevent further acid accumulation in the blood. A patient with metabolic acidosis will often demonstrate a rapid breathing pattern, known as Kussmaul breathing.In addition to measuring the patient's respiratory rate, the examiner will observe the patient's breathing pattern: Pectus carinatum, sternum protruding from the chest.Pectus excavatum, sternum sunken into the chest.Barrel chest, bulging out of the chest wall normal in children typical of hyperinflation seen in chronic obstructive pulmonary disease (COPD).Scoliosis, abnormal lateral curvature of the spine.Kyphosis, abnormal anterior-posterior curvature of the spine.The anterior and posterior chest wall are also inspected for any abnormalities, which may include: An increased jugular venous pressure, indicating possible right heart failure.Decreased chest–chest movement on the affected side.Diaphragmatic breathing, paradoxical movement of the diaphragm outwards during inspiration.Accessory muscle use, including the scalene and intercostal muscles.Cyanosis, a bluish tinge of the extremities (peripheral cyanosis), or of tongue (central cyanosis).Īfter obtaining the patient's respiratory rate, the examiner looks for any signs of respiratory distress, which may include:
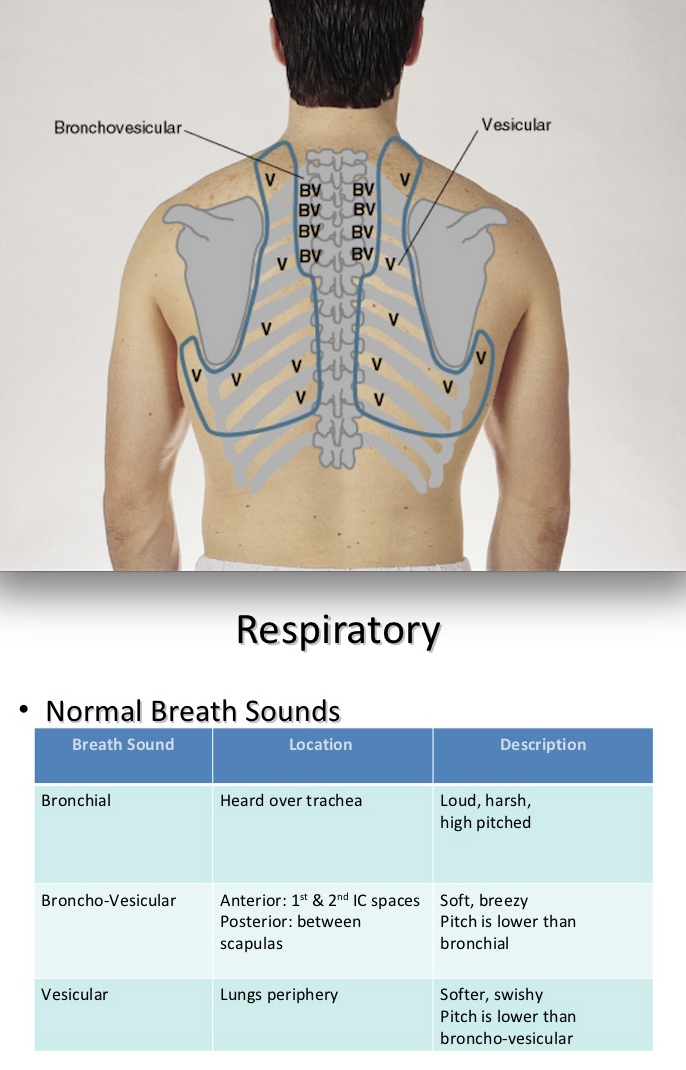

Adults normally breathe about 14 to 20 times per minute, while infants may breathe up to 44 times per minute. This is typically conducted under the pretext of some other exam, so that the patient does not subconsciously change their baseline respiratory rate, as they might do if they were aware of the examiner observing their breathing.

The examiner then estimates the patient's respiratory rate by observing how many times the patient breathes in and out within the span of one minute. These fields are intended to correlate with the lung lobes and are thus tested on the anterior (front) and posterior (back) chest walls. In order to listen to the lungs from the back the patient is asked to move their arms forward to prevent the scapulae (shoulder blades) from obstructing the upper lung fields. Stages Īfter positioning in which the patient sits upright with their arms at the side, with the chest clear of clothing, the four stages of the examination can be carried out. The four steps of the respiratory exam are inspection, palpation, percussion, and auscultation of respiratory sounds, normally first carried out from the back of the chest. Part of physical exam(or when a respiratory problem is present)Ī respiratory examination, or lung examination, is performed as part of a physical examination, in response to respiratory symptoms such as shortness of breath, cough, or chest pain, and is often carried out with a cardiac examination.
